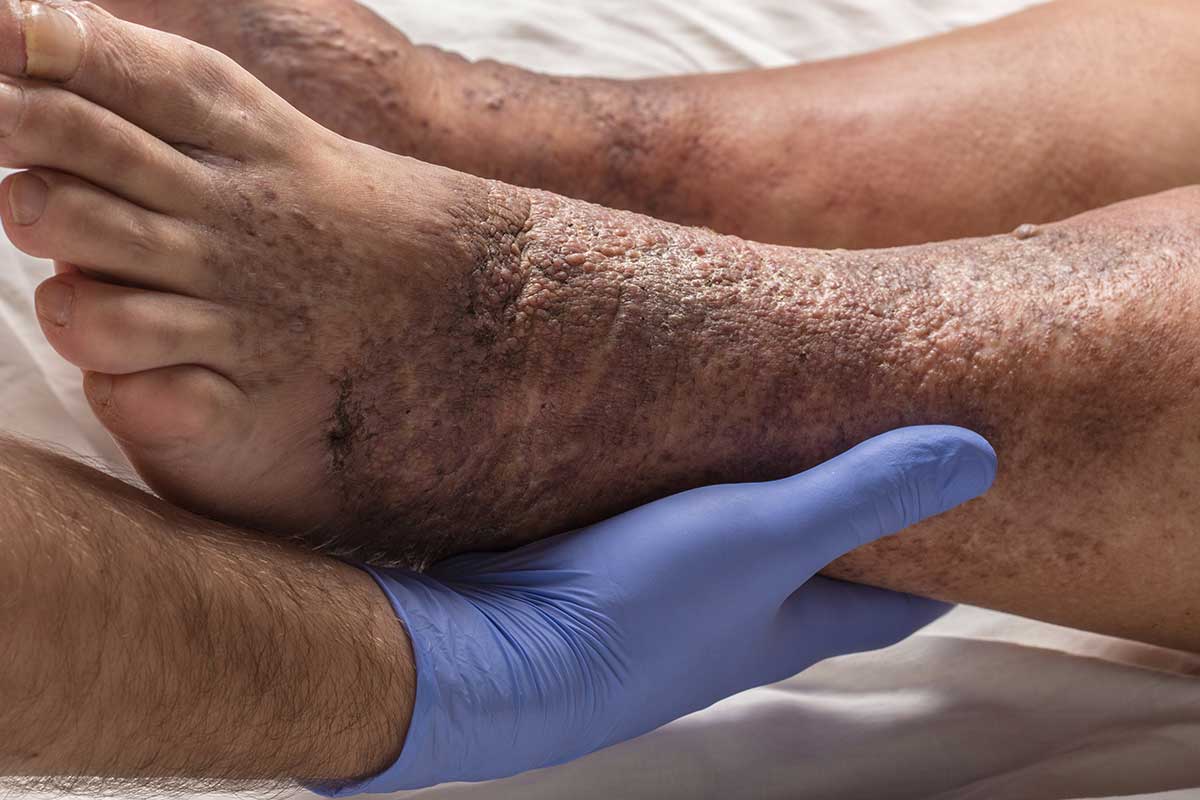
What is Cellulitis?
Cellulitis is an infection of the skin and the tissues just beneath the skin. It often leads to swelling, redness, and pain. While cellulitis itself is not usually life-threatening, it can become severe and spread to deeper tissues if left untreated. Early diagnosis and treatment are key to preventing complications such as abscess formation, sepsis, or the spread of the infection to other parts of the body.
Symptoms of Cellulitis
The symptoms of cellulitis can vary depending on the severity of the infection. In most cases, cellulitis presents with the following:
- Redness and Swelling
The skin affected by cellulitis may appear red and swollen. The redness often spreads rapidly and may be warm to the touch.
- Pain or Tenderness
The infected area is usually painful and tender. You may feel discomfort even without touching the affected skin.
- Fever and Chills
As cellulitis is an infection, it may cause a fever, chills, and general malaise. If the infection is severe, these symptoms can become more pronounced.
- Skin Tightness and Blisters
The affected area may feel tight or stretched. In some cases, blisters or pustules may form on the skin, particularly if the infection is severe.
- Warmth to the Touch
The skin over the infected area may feel warm or hot to the touch due to inflammation and increased blood flow.
- Swollen Lymph Nodes
In more severe cases, cellulitis can cause swelling in the lymph nodes closest to the infection, as the body attempts to fight off the infection.
Causes of Cellulitis
Cellulitis is caused by bacteria that enter the skin through breaks, cuts, or wounds. The most common bacteria responsible for cellulitis are:
- Streptococcus
Streptococcus is a group of bacteria that can enter the body through minor skin injuries like cuts, abrasions, or insect bites. This bacterium is often associated with more superficial skin infections.
- Staphylococcus (including MRSA)
Staphylococcus aureus is another type of bacteria that can cause cellulitis, especially in more severe cases. A subtype of this bacterium, methicillin-resistant Staphylococcus aureus (MRSA), is resistant to many antibiotics, making infections harder to treat.
Risk Factors for Cellulitis:
Certain conditions can make you more susceptible to developing cellulitis. These include:
- Weakened immune system (due to diseases like diabetes, cancer, or HIV/AIDS)
- Chronic skin conditions like eczema or athlete’s foot
- Lymphedema or other conditions that impair lymphatic drainage
- Previous skin injury or surgery that disrupts the skin barrier
- Obesity
- Poor circulation, particularly in the legs
- Intravenous drug use that involves needle injection into the skin
- Insect bites or animal scratches
Treatment Options for Cellulitis
The treatment for cellulitis generally involves antibiotics to treat the underlying bacterial infection. Depending on the severity of the infection, treatment may be done on an outpatient basis or require hospitalization.
- Antibiotics
The mainstay of cellulitis treatment is antibiotics. If the infection is mild, your doctor may prescribe oral antibiotics such as:
- Penicillin or Amoxicillin
- Cephalexin
- Clindamycin
- Doxycycline
For more severe infections or those caused by MRSA, stronger antibiotics may be necessary, such as:
- Trimethoprim-sulfamethoxazole (Bactrim)
- Clindamycin
- Vancomycin (administered intravenously)
- Hospitalization and Intravenous Antibiotics
In cases where the infection is severe, spreading quickly, or not responding to oral antibiotics, hospitalization may be required. Patients will be given intravenous (IV) antibiotics to quickly treat the infection. Hospitalization may also be needed for individuals with other health problems, such as diabetes or a weakened immune system.
- Pain Relief and Anti-inflammatory Medications
Over-the-counter pain relievers such as acetaminophen (Tylenol) or ibuprofen can help relieve pain, swelling, and fever associated with cellulitis. Anti-inflammatory medications may be prescribed to reduce the swelling and inflammation.
- Elevation and Rest
Resting and elevating the affected area can help reduce swelling. If cellulitis affects the legs, elevating the leg above heart level may promote fluid drainage and alleviate discomfort.
- Incision and Drainage (for Abscesses)
If the cellulitis results in a localized abscess or collection of pus, your healthcare provider may need to drain the abscess. This procedure is typically done under local anesthesia and helps to alleviate pain and speed up recovery.
- Wound Care and Hygiene
Good wound care is essential for preventing the spread of infection. If there is an open wound or injury, clean it with mild soap and water, apply an antibiotic ointment, and cover it with a clean bandage. Keeping the wound clean and covered will help prevent additional bacteria from entering and causing further infection.
Complications of Cellulitis
If left untreated or if treatment is delayed, cellulitis can lead to more severe complications. These include:
- Sepsis: A life-threatening condition where the infection spreads throughout the body.
- Abscess formation: A localized collection of pus that may require surgical drainage.
- Chronic lymphatic problems: Prolonged or recurrent cellulitis can damage the lymphatic system, leading to chronic swelling (lymphedema).
- Deep tissue infection: In rare cases, cellulitis can spread to deeper tissues and cause conditions like necrotizing fasciitis (a rapidly progressing soft tissue infection).
Prevention of Cellulitis
While cellulitis cannot always be prevented, there are steps you can take to reduce your risk:
- Practice good hygiene: Clean your skin regularly, especially if you have cuts, scrapes, or open wounds.
- Keep wounds covered: Apply a clean bandage to cuts, scrapes, or insect bites to prevent bacteria from entering.
- Moisturize skin: Dry, cracked skin is more susceptible to infection, so keep your skin hydrated with lotion.
- Manage chronic conditions: Proper management of diabetes, lymphedema, or any other underlying conditions can help prevent cellulitis.
Avoid scratching insect bites: If you have an insect bite or scrape, resist scratching to prevent introducing bacteria.
Conclusion
Cellulitis is a common bacterial infection that can cause significant discomfort and lead to severe complications if not treated promptly. Understanding the symptoms, causes, and treatment options is crucial for early intervention. With appropriate antibiotic treatment, rest, and care, most people with cellulitis can make a full recovery.
If you suspect you have cellulitis, it’s important to seek medical attention as soon as possible to avoid complications. Early treatment with antibiotics can help prevent the infection from spreading and ensure a quicker recovery.